In a new report written by the Lancet Commission on Investing in Health (the CIH), launched at last week’s Alma Ata at 40 meeting, the CIH draws on evidence from the third edition of the Disease Control Priorities (DCP3) to define essential universal health coverage (EUHC). DCP3 was a 7-year international collaboration that synthesized evidence on the most effective way to tackle priority health conditions in low-income countries (LICs) and middle-income countries (MICs). A key output of DCP3 was a set of 21 essential packages of interventions, each one aimed at a different health priority (e.g. reproductive health, pandemic preparedness). As the CIH notes in the Alma Ata at 40 report: “Interventions were included in these 21 packages if they provided good value for money, were feasible to implement in LICs and MICs, and addressed a relevant burden of disease.”
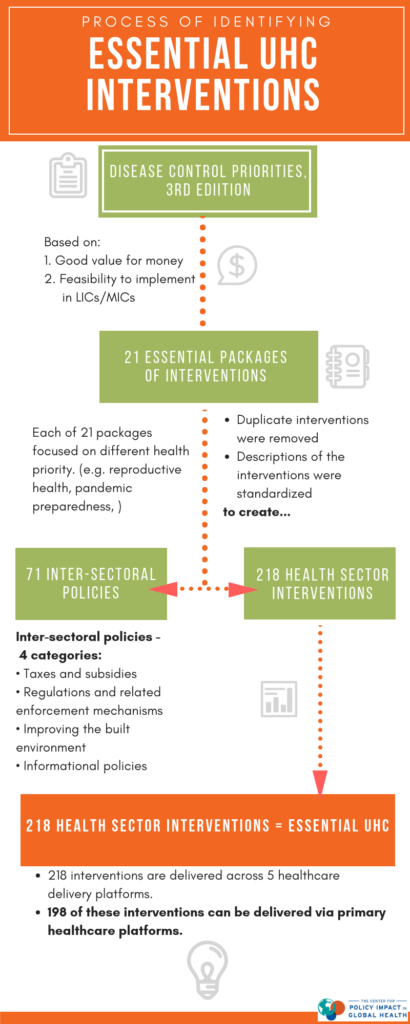
These 21 packages were the starting point for defining EUHC (Figure 1). Any duplicate interventions across the 21 packages were removed and the descriptions of the interventions were standardized. Finally, two lists were created: (i) a list of 71 inter-sectoral policies, grouped across four broad categories (taxes and subsidies; regulations and related enforcement mechanisms; improving the built environment; and informational policies); and (ii) a list of 218 health sector interventions, which are termed EUHC.
These 218 interventions in EUHC are delivered across five delivery platforms:
- Population based (public health) health interventions (n=13)
- Community based health interventions (n=59)
- Health centers (n=68)
- First level hospitals (n=58)
- Referral and specialty hospitals (n=20).
For the Alma Ata report, the CIH defines primary healthcare as “health care that centers on the platforms required to deliver essential interventions close to the population,” i.e. the first four of the above platforms. In other words, all but 20 of the 218 EUHC interventions can be delivered in primary care.
What kind of impact would the scale up of EUHC have? The CIH has shown that if these 218 interventions reached everyone who needed them, the “40 by 30” target in Sustainable Development Goal 3 would be reached (i.e., reducing premature mortality from all causes in people aged under 70 years by 40 percent by 2030).
In their recent commentary for Global Health NOW, Gavin Yamey and David Watkins, the joint first authors of the CIH’s Alma Ata report, comment on the financial feasibility of EUHC scale-up. They ask:
“Is EUHC affordable? With anticipated economic growth, by 2030 most middle-income countries will be able to afford EUHC delivered through primary health care. However, many low-income countries could struggle unless their macroeconomic conditions improve; these countries are likely to need external financing for years to come.”
But they also note that even scaling up the 218 EUHC interventions, representing the most cost-effective interventions, will require a massive increase in domestic spending on health. On average, it will cost, say Yamey and Watkins, “about $100 per person—much higher than the $20 per person that governments are spending across low- and lower middle-income countries.”
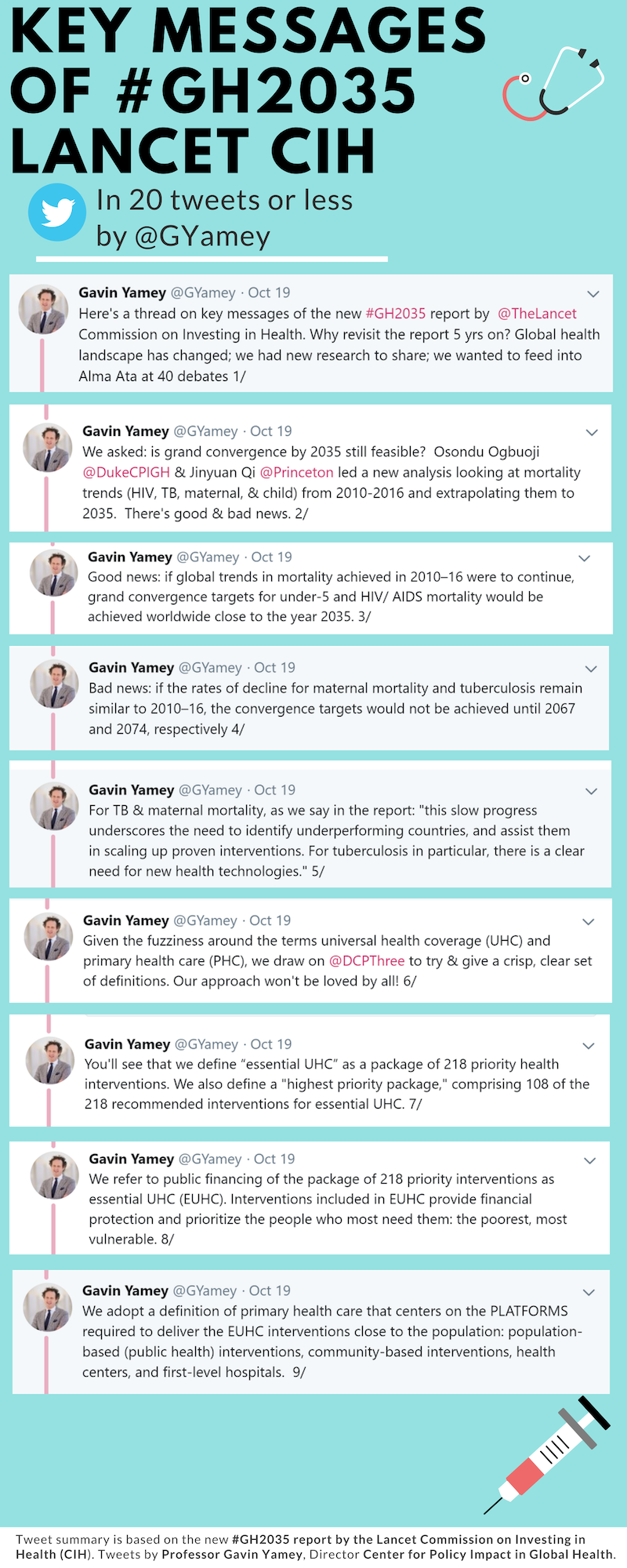
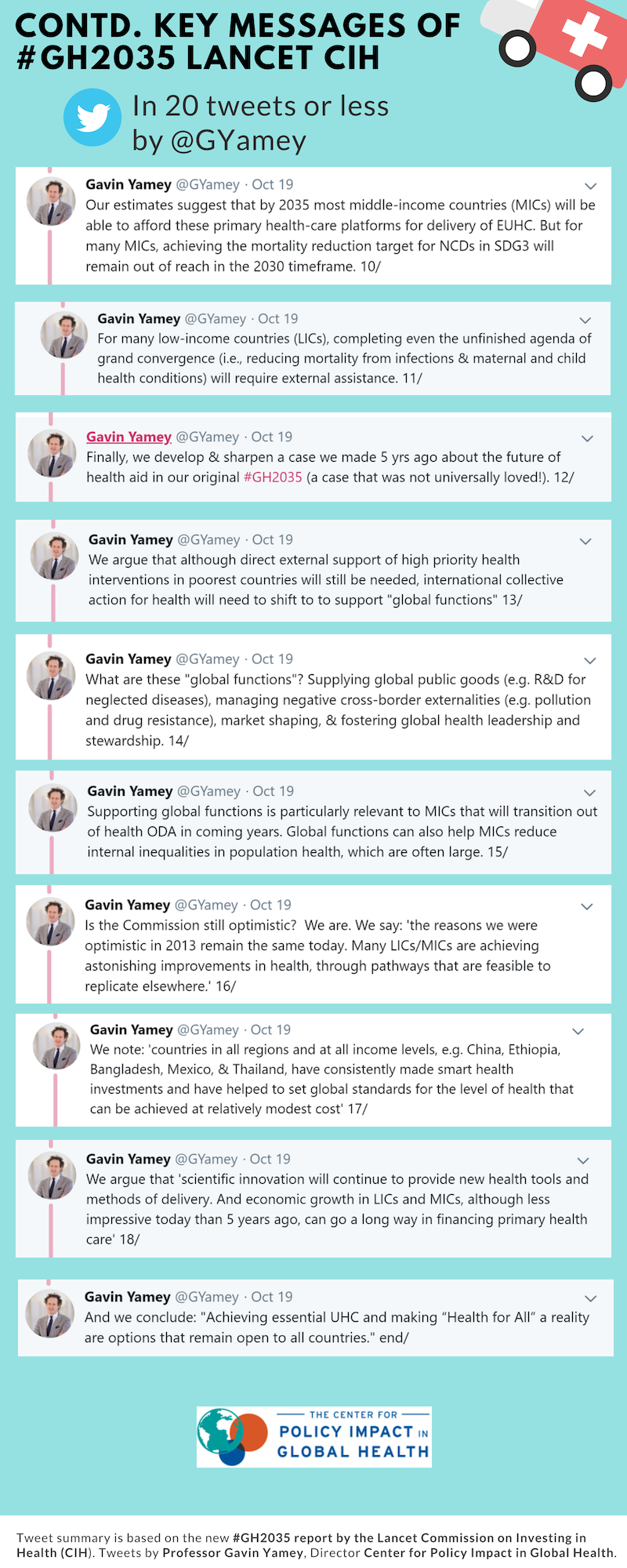
Yamey tweeted out a summary of the 19 key messages of the CIH’s Alma Ata report (Figure 2), which sparked an important discussion about the pros and cons of EUHC. Take a look at this intriguing debate between Yamey and public health physician Kumanan Rasanathan, who works for the WHO in Cambodia. For example, Rasanathan asks, “isn’t ‘essential UHC’ uncomfortably close to ‘selective PHC’? And a bit of an oxymoron?” Yamey notes that the list of interventions includes surgery, palliative care, and rehabilitation, saying “Right now, the fuzziness around UHC is paralyzing, no? Essential UHC is a way of saying: what would an effective package of pro-poor interventions look like.”
This debate is unlikely to end any time soon. The CIH hopes that by putting EUHC on the table, countries have an evidence-based package that can be contextualized and adapted for local needs.
Author:
Shashika Bandara, Policy Analyst, Center for Policy Impact in Global Health, Duke Global Health Institute. (tweets @shashikaLB)
